
Osteochondrosis is a disease in which degenerative-dystrophic changes in the cartilaginous tissues of the spine are diagnosed, which are also associated with disturbances in the structure and function of the intervertebral discs.Depending on the location of the damaged tissue, osteochondrosis of the cervical, thoracic and lumbar regions is distinguished.
According to medical statistics, symptoms of osteochondrosis are observed in 50-90% of the population.The average age of onset of osteochondrosis is 30-35 years.Under adverse conditions, signs of osteochondrosis may appear earlier, especially in the case of long-term uneven loading of the back, legs and the consequences of injuries.
What is osteochondrosis?
Osteochondrosis is a disease of the spine in which degenerative and dystrophic changes of the intervertebral discs occur.With the development of osteochondrosis, degenerative-dystrophic changes spread to the tissues of the vertebrae.
The main symptom of osteochondrosis is pain in the neck, back and lumbar region;as it progresses, the pain "radiates" into the arms, chest, shoulders, and thighs.With the negative dynamics of osteochondrosis, atrophy of muscle tissue, sensory disturbances and dysfunctions of internal organs begin, which are caused by their compression and displacement.In the absence of timely treatment, osteochondrosis becomes incurable.
Causes of osteochondrosis
The main factor in the development of osteochondrosis is uneven loading of the spine.A common cause of incorrect load distribution is carrying the bag on one shoulder or in one hand, the wrong sitting position, sleeping on too soft a mattress, high pillow and wearing anatomically inappropriate shoes.
Other risk factors include physical inactivity, sedentary lifestyle, overweight, back and lower limb injuries, flat feet and other disorders of the musculoskeletal system, as well as age-related degenerative processes resulting from age-related changes in blood supply to the spine.
The following factors can also play a role in the etiology of osteochondrosis:
- physical overload of the body;
- neuro-emotional exhaustion;
- metabolic disorders, poisoning, diseases of the gastrointestinal tract, which prevent the complete absorption of nutrients;
- occupational risks, especially when working on vibrating platforms;
- genetic predisposition;
- bad posture during the period of active growth, scoliosis;
- wearing uncomfortable shoes (tight, heels);
- prolonged and/or regular dehydration;
- poor diet, hypovitaminosis;
- smoking;
- pregnancy, especially multiple pregnancy, combined with an underdeveloped musculo-ligamentous apparatus (due to the shift of the body's center of gravity).
Stages of development of osteochondrosis
Osteochondrosis goes through four stages in the dynamics of the disease:
- Stage 1 (degree) osteochondrosis is characterized by the initial stage of pathology in the nucleus pulposus of the intervertebral disc.Due to excessive load, the process of desiccation (drying) of the core begins, which leads to a decrease in the height of the plate and the appearance of cracks in the fibrous ring.Symptoms at this stage are usually absent;slight discomfort may occur during prolonged uncomfortable static positions or during active movement;
- in stage 2, a decrease in the height of the discs leads to a decrease in the distance between the vertebrae and a sagging of the spinal muscles and ligaments.This causes increased mobility of vertebrae with affected discs, which is dangerous due to their displacement or slippage.In the second stage of the disease, discomfort and pain appear, especially with certain types of loads, movements, positions;
- The 3rd stage (degree) of osteochondrosis is characterized by the development of prolapses and protrusions of the intervertebral discs, and may be accompanied by the development of subluxations and/or arthrosis of the intervertebral joints.With certain types of movement, patients may experience stiffness, lack of movement, and tingling and numbness in the limbs.At this stage of osteochondrosis, the pain is clearly felt in the back, neck, lumbosacral region or coccyx, depending on the location of the affected discs;
- In the 4th stage of osteochondrosis, the body tries to correct the consequences of the hypermobility of the vertebrae and adapt to the damaged function of the spinal column.Osteophytes, new bone formations, improve the fixation of the vertebrae, they are formed at the contact points of the vertebrae.However, in some cases, osteophytes can pinch the nerves and injure the vertebrae.Fibrous ankylosis begins in the intervertebral discs and joints.In the absence of microtraumas and pinched nerve roots, the symptoms of the disease are alleviated.
Symptoms of osteochondrosis

The main symptoms of osteochondrosis are discomfort and/or pain in the neck and back.The severity of the sensations and the presence of additional symptoms depend on the stage of the disease.When examining the patient and collecting the anamnesis, the specialist makes a primary diagnosis, which indicates the presence of osteochondrosis with a visually detectable curvature of the spine in the transverse or longitudinal plane of the spine.Pathologies of the intervertebral discs of the cervical and lumbar spine are much more common than degenerative and dystrophic changes of the sternum.
Symptoms of osteochondrosis are periodic or permanent back fatigue felt by the patient, mild or severe pain, depending on the stage of the disease.The pain can be localized in the neck, back, chest, shoulder girdle, making it difficult and limiting the movement of the upper limbs.
The clinical picture of osteochondrosis largely depends on the localization of the pathology, the degree of development of the process and the individual characteristics of the patients.Pathology of the intervertebral discs, displacements, protrusions, hernias and the growth of osteophytes have various consequences.The most common are disorders of normal tissue blood circulation, pinching of nerve endings, spinal canal dysfunction, edema, and fibrosis of tissues and structures.Such consequences can be accompanied by many different symptoms, which can lead to the wrong diagnosis of diseases.
The most common and characteristic symptoms of osteochondrosis are the following:
- pain in the back, neck, lower back, shoulder girdle, ribs;
- discomfort, stiffness in body movements, which occurs in certain body positions, bending, turning, increased muscle tension;
- a feeling of numbness in the upper and lower limbs;
- muscle and joint discomfort, muscle spasms;
- headache, dizziness, increased fatigue;
- pain in the area of the heart;
- impaired hand sensitivity;
- muscle hypotonia.
Symptoms of osteochondrosis vary depending on the location of the pathology:
- with osteochondrosis of the cervical spine, pain in the neck, arms and shoulder girdle dominates, radiating to the scapula and shoulder area;headache, dizziness, flashing "spots" or spots in front of the eyes, and tinnitus;
- if the thoracic spine is affected, the pain is localized in the chest, heart, inner surface of the shoulder, in the armpit, breathing discomfort also occurs, shortness of breath is possible;
- Osteochondrosis of the lumbosacral spine is manifested by low back pain radiating to the legs, upper thighs or pelvic organs, often accompanied by sexual dysfunction.
Superficial symptoms - back fatigue, pain - can indicate not only the presence of osteochondrosis, but also the addition of other diseases or the development of other pathological processes and disorders that are not related to the degeneration of the intervertebral discs.The diagnosis of "osteochondrosis" can only be made by a specialist, and self-medication of such symptoms is unacceptable.
Classification of osteochondrosis
Types of osteochondrosis are distinguished according to several principles.Depending on the location of the pathology, osteochondrosis of the neck, chest, lumbar, sacrum or mixed, combined diseases is distinguished.According to the clinical manifestations, osteochondrosis with different localization is divided into subtypes depending on the identified symptoms and the overall clinical picture.
Osteochondrosis of the cervical spine:
- depending on the type of reflex syndrome, cervicalgia, cervicocranialgia, cervicobrachialgia are identified with different manifestations (vegetative-vascular, neurodystrophic, muscle-tonal);
- if the test result for radicular syndrome is positive, discogenic damage to the roots of the cervical spine is diagnosed.
Thoracic level pathology includes:
- in case of reflex syndromes - thoracalgia with vegetovisceral, neurodystrophic or muscle-tonal manifestations;
- with radicular - discogenic changes in the roots of the chest region.
In the case of osteochondrosis at the lumbosacral level, the following are diagnosed:
- depending on the type of reflex syndrome - lumbago (lumbago), lumbodynia, lumboischialgia with vegetative-vascular, neurodystrophic or muscle-tonal manifestations;
- radicular syndrome indicates discogenic damage to the roots of the lumbosacral region;
- radicular vascular syndrome indicates radiculoischaemia.
Diagnosis of osteochondrosis
Instrumental examination methods are used to establish the diagnosis:
- X-ray examination of the spine;
- myelography;
- neurological examination of sensitivity and reflexes.
Additional methods prescribed for distinguishing and clarifying the stage of diagnosis and pathology are as follows:
- computed tomography (CT) of the spine;
- nuclear magnetic resonance (NMR);
- magnetic resonance imaging (MRI).
Directions for the treatment of osteochondrosis
The treatment is based on an integrated approach and, depending on the stage, takes 1-3 months of intensive therapy and 1 year of supportive measures to consolidate the result and prevent relapses.
The therapy of the disease of osteochondrosis is carried out in two directions, depending on the degree of osteochondrosis and the patient's state of health.Conservative treatment of the disease consists of taking medicines and performing exercises.Surgical treatment cannot be the method of first choice in almost all situations, and is prescribed in the absence of positive dynamics or disease progression against the background of long-term conservative therapy.
In addition to medical therapeutic methods, general recommendations for osteochondrosis should be followed: follow a diet, take the necessary measures for rehabilitation.
Conservative treatment of osteochondrosis
Conservative therapy is aimed at relieving pain, normalizing the function of the spine and preventing negative changes.
Conservative treatment of osteochondrosis includes the following types of therapy:
- drug therapy.Medicines for the treatment of osteochondrosis are used to alleviate pain syndromes, inflammatory processes in tissues, and normalize the body's metabolic processes.In case of severe pain syndrome, it is recommended to use drug blockades of nerve endings, which also help to reduce the severity of muscle tone syndrome.The following types of blockades are distinguished: trigger point blockade, intraosseous, facet, paravertebral, epidural;
- physiotherapy methods.Physiotherapy procedures help reduce pain, increase the effect of drugs, and are also used during the rehabilitation period.The most common uses are ultrasound waves, magnetic fields, low-frequency currents, and laser beams;
- methods of physical therapy (physiotherapy) and kinesitherapy.Regular and correct execution of special exercises helps to correct posture, strengthen the ligaments and ligaments, normalize muscle function, reduce compression of nerve fibers and prevent complications of osteochondrosis.The methods of movement therapy and kinesitherapy procedures are aimed at normalizing metabolic processes, restoring proper nutrition of the intervertebral discs, restoring the location of the vertebrae and the discs between them, and evenly distributing the load in the musculoskeletal system;
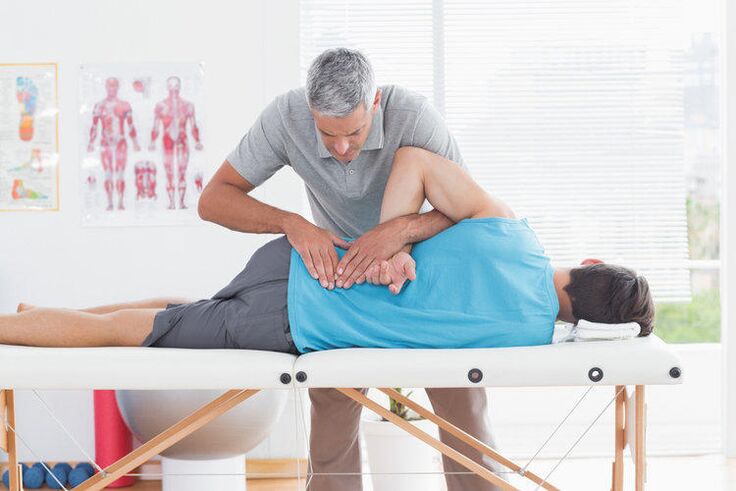
- massage.Manual massage techniques are used to improve tissue blood supply, relieve muscle spasms and tension, and generally improve circulation.Hydromassage, as a form of therapeutic activity, helps to normalize the functioning of the body's nervous system in addition to the listed effects;
- manual therapy.Manual therapy methods are selected individually.The targeted effect on the musculoskeletal system of the body improves blood circulation, lymph circulation, improves metabolism, helps to correct the mobility of the musculoskeletal system, strengthens the immune system, and serves to prevent the complications of osteochondrosis;
- traction therapy(traction) of the spine with special equipment.The aim of the manipulations is to increase the intervertebral space to normal parameters and to correct the structural abnormalities of the spinal column.
Osteochondrosis: drug therapy
In the treatment of osteochondrosis, the drugs aim to reduce the severity of symptoms, improve the blood supply and regeneration of tissues.Osteochondrosis cannot be cured by taking medicines alone;therapy should be combined, including exercise, diet, and preventive measures.
In the absence of pronounced dystrophic changes and pain, it is considered unjustified to take medicines without a prescription from a specialist.
Medicines for pain relief and osteochondrosis treatment:
- anti-inflammatory group;
- antioxidant preparations: vitamin C (as ascorbic acid), E (tocopherol acetate), N (thioctic acid);
- means to improve tissue blood supply, B vitamins (mainly B3);
- preparations for the regeneration and/or prevention of cartilage tissue, hyaluronic acid.
Medicines can be prescribed in the form of both ointments and pain-relieving creams, as well as for oral administration and injections.
In case of acute complications, drugs are used to block the nerve endings.
Osteochondrosis: dietary nutrition of the patient
The basic principles of the diet are based on the need to improve metabolic processes, saturate the body with essential nutrients, vitamins, and minerals, and include foods rich in antioxidants, polyunsaturated fatty acids, and compounds that promote the regeneration of cartilage tissue.The purpose of the recommended drinking regimen for osteochondrosis is to prevent the body from drying out, which can negatively affect the affected tissues.Eat in small portions, 5-6 times a day.
The basis of the diet is milk and fermented milk products, lean meats, poultry, fish, fresh vegetables, fruits, nuts and seeds, cereals, mushrooms.It is especially recommended to include meat and fish jellies, jellied meats, and gelatinous foods in the diet, and use extra virgin olive oil without heat treatment (for dressing salads).
Preferred food processing methods: steaming, baking, boiling.Limit the consumption of flour and confectionery products, fatty foods, spicy, salty foods and spices, canned and smoked foods, strong broths, legumes, sugar and fruits with a high sugar content (grapes).During the day, you should drink at least 1.5 liters of liquid, giving preference to clean and mineral water, dried fruit compotes, unsweetened fruit drinks and herbal teas.You should limit the amount of strong black tea, coffee, sweet carbonated drinks and alcohol.
Complications of osteochondrosis
Non-compliance with the prescribed treatment, long-term avoidance of the doctor and lack of treatment of osteochondrosis contribute to the progression of the disease and lead to the development of complications, pathologies and new diseases, such as:
- intervertebral disc herniation (spinal hernia);
- protrusion;
- kyphosis;
- radiculitis;
- salt deposits in the intervertebral space;
- spinal cord stroke;
- decrease in muscle mass of the limbs, muscle atrophy due to blood supply disorders;
- paralysis of the lower limbs.
Despite the fact that osteochondrosis of the 4th degree can occur without serious symptoms and pain, advanced osteochondrosis is the most dangerous for the development of serious complications and can lead to disability of the patient.
Prevention of osteochondrosis

The causes of osteochondrosis are mainly related to the lack of attention to the needs of the body, improper nutrition and excessive stress on the body.In order to prevent pathological changes in the spine and control the dynamics of existing osteochondrosis, it is recommended to follow the general principles of a healthy lifestyle:
- eliminating the possibility of physical inactivity: moderate sports: exercise, running, swimming, cycling, skiing, gymnastics, non-contact wrestling, etc.;
- During work or other activities that require long periods of static posture, you should take a warm-up break every 45 minutes to restore blood circulation.If you have to sit for a long time, choose suitable chairs, chairs that support the spine, ensure compliance with the standards for the position of hands on the table, feet on the floor or a special stand, learn to maintain posture (straight back, relaxed shoulders);
- for night sleep, you should choose an elastic, preferably orthopedic mattress with a flat surface, avoid high or too flat pillows;
- if necessary, lift and/or transport heavy objects, avoid jerking when lifting weights from a semi-squatting position, use special belts to support the lower back;
- choosing the right orthopedic shoes: with the right width for the feet, without high heels and changing them in time helps to reduce the load on the spine, this is especially important for women during childbearing.In the summer, don't ignore the opportunity to walk barefoot on uneven surfaces;it strengthens the leg muscles and relieves the tension of the musculoskeletal system;
- A proper diet and drinking regimen contributes to general health and helps maintain normal metabolism;
- If you are prone to increased emotionality, anxiety associated with muscle spasm stress reaction, it is worth learning relaxation methods, as well as regularly participating in restorative massage courses.





































